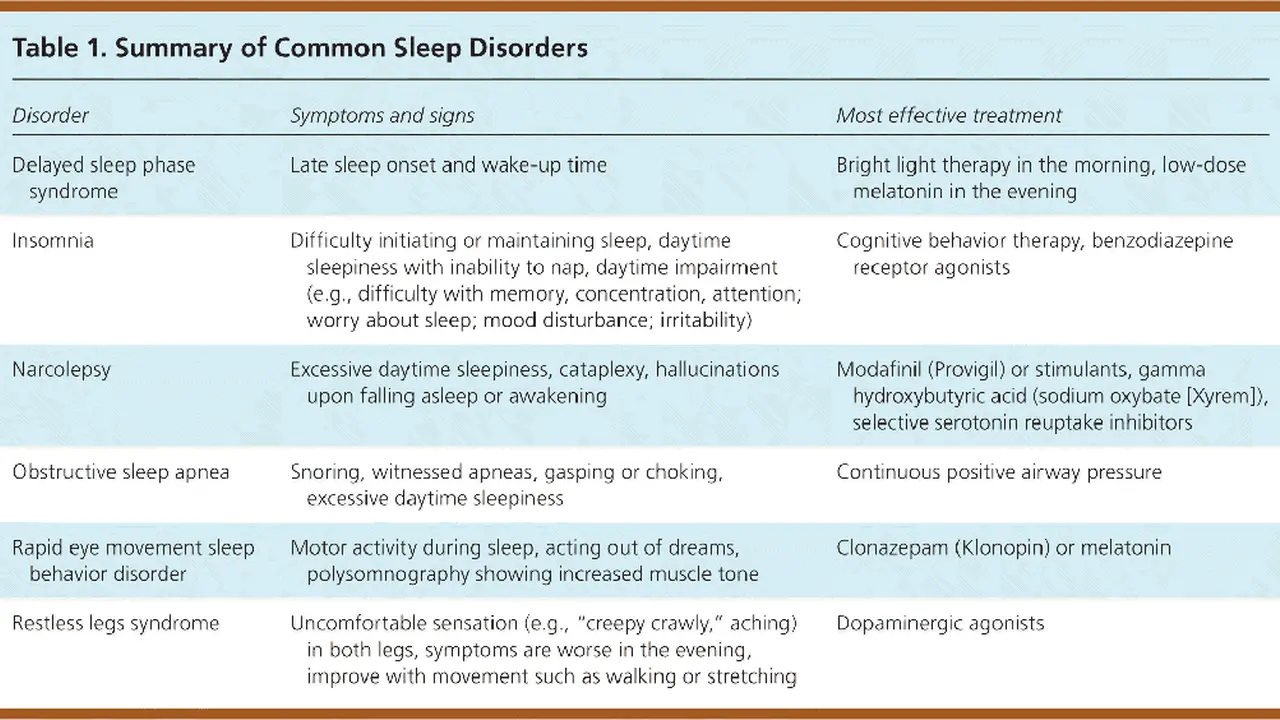
Sleep Disorder Diagnosis Process
Learn about the diagnostic procedures for various sleep disorders. Prepare for your sleep study and consultation.
Learn about the diagnostic procedures for various sleep disorders. Prepare for your sleep study and consultation.
Sleep Disorder Diagnosis Process
Hey there, ever wondered why you're always tired, even after what feels like a full night's sleep? Or maybe your partner complains about your snoring, or you find yourself nodding off during the day? These could be signs of a sleep disorder, and getting a proper diagnosis is the first crucial step towards feeling better. It's not just about feeling sleepy; untreated sleep disorders can seriously impact your overall health, mood, and quality of life. So, let's dive into how sleep disorders are diagnosed, what you can expect during the process, and some of the tools and tests involved.
Initial Consultation Understanding Your Sleep Issues
The journey to diagnosis usually begins with a visit to your primary care doctor or a sleep specialist. This initial consultation is super important because it's where you'll share your sleep history and symptoms. Don't hold back! Be as detailed as possible about what you're experiencing. Your doctor will likely ask you a bunch of questions, such as:
- What are your main sleep complaints? (e.g., difficulty falling asleep, staying asleep, excessive daytime sleepiness, snoring, restless legs)
- How long have you been experiencing these symptoms?
- What's your typical sleep schedule like? (bedtime, wake-up time, naps)
- Do you have any pre-existing medical conditions?
- What medications are you currently taking?
- Do you consume caffeine, alcohol, or nicotine, and how much?
- What's your daily routine like? (work, exercise, stress levels)
- Has anyone observed anything unusual about your sleep? (e.g., gasping for air, loud snoring, restless movements)
They might also ask you to keep a sleep diary for a week or two before your appointment. This diary helps track your sleep patterns, habits, and any symptoms you experience. It's a great way to provide concrete data rather than just relying on memory.
Physical Examination and Medical History Sleep Health Assessment
Beyond the questions, your doctor will perform a physical examination. This isn't just a routine check-up; they'll be looking for specific signs that might point to a sleep disorder. For instance, they might check your throat and nasal passages for any obstructions that could contribute to sleep apnea. They'll also assess your overall health, looking for conditions that often co-exist with sleep disorders, like high blood pressure, obesity, or thyroid issues. Your complete medical history, including any family history of sleep disorders, will also be taken into account.
Sleep Studies The Gold Standard for Diagnosis
If your doctor suspects a sleep disorder, they'll likely recommend a sleep study, also known as a polysomnogram (PSG). This is the most comprehensive way to diagnose many sleep disorders. There are a couple of main types:
In Lab Polysomnography Comprehensive Sleep Analysis
This is the classic sleep study where you spend a night at a sleep clinic or hospital. It might sound a bit intimidating, but it's usually a comfortable, private room. During the PSG, various sensors are attached to your body to monitor different physiological functions while you sleep. These include:
- Electroencephalogram (EEG): Measures brain waves to identify sleep stages (REM, non-REM) and detect sleep-related brain activity.
- Electrooculogram (EOG): Records eye movements, which are crucial for identifying REM sleep.
- Electromyogram (EMG): Monitors muscle activity, particularly in your chin and legs, to detect restless leg syndrome or other movement disorders.
- Electrocardiogram (ECG/EKG): Tracks your heart rate and rhythm.
- Respiratory Effort Sensors: Placed around your chest and abdomen to measure breathing effort.
- Nasal Airflow Sensors: Detect airflow through your nose and mouth to identify pauses in breathing.
- Pulse Oximetry: A clip on your finger measures the oxygen levels in your blood. Drops in oxygen can indicate sleep apnea.
- Video Recording: Often used to observe body movements, snoring, and any unusual behaviors during sleep.
All this data is collected and analyzed by a sleep technologist and then interpreted by a sleep physician. It provides a detailed picture of your sleep architecture, breathing patterns, heart activity, and movements throughout the night.
Home Sleep Apnea Testing HST Convenient Sleep Monitoring
For suspected cases of obstructive sleep apnea (OSA), a home sleep apnea test (HST) might be an option. This is a more convenient and less expensive alternative to an in-lab PSG. You'll be given a portable device to use in your own bed. While HSTs are great for diagnosing OSA, they don't provide as much detailed information as an in-lab PSG, as they typically only measure:
- Nasal airflow
- Respiratory effort
- Blood oxygen levels
- Heart rate
HSTs are generally not suitable for diagnosing other complex sleep disorders like narcolepsy or restless legs syndrome, as they don't monitor brain waves or detailed body movements.
Other Diagnostic Tests Specific Sleep Disorder Assessments
Depending on your symptoms and the initial findings, your doctor might recommend additional tests:
Multiple Sleep Latency Test MSLT Daytime Sleepiness Evaluation
If excessive daytime sleepiness is a major concern, an MSLT might be performed the day after an in-lab PSG. This test measures how quickly you fall asleep during the day in a quiet environment. You'll have several scheduled nap opportunities (usually five, 20 minutes each, spaced two hours apart). It helps diagnose conditions like narcolepsy or idiopathic hypersomnia.
Maintenance of Wakefulness Test MWT Alertness Measurement
The MWT is similar to the MSLT but measures your ability to stay awake during the day in a quiet environment. It's often used to assess the effectiveness of treatment for sleep disorders or to determine if someone is fit to perform certain tasks, like driving, safely.
Actigraphy Wearable Sleep Tracking
Actigraphy involves wearing a small device, usually on your wrist, that records your movement patterns over several days or weeks. It's like a fancy fitness tracker but specifically for sleep. It can help assess your sleep-wake cycles, identify circadian rhythm disorders, and provide a long-term view of your sleep patterns in your natural environment. While not a diagnostic tool on its own, it provides valuable supplementary data.
Interpreting the Results Understanding Your Diagnosis
Once all the tests are complete, a sleep physician will analyze the data and provide a diagnosis. They'll explain what the results mean for you and discuss potential treatment options. This might involve lifestyle changes, continuous positive airway pressure (CPAP) therapy for sleep apnea, medications, or other interventions. It's a collaborative process, so don't hesitate to ask questions and ensure you understand your diagnosis and the proposed treatment plan.
Recommended Products and Tools for Sleep Disorder Management
While diagnosis is key, managing sleep disorders often involves specific products and tools. Here are some common ones, with comparisons and typical price ranges:
CPAP Machines for Sleep Apnea Breathing Support
For obstructive sleep apnea, CPAP (Continuous Positive Airway Pressure) machines are the most common and effective treatment. They deliver a continuous stream of air through a mask worn during sleep, keeping your airway open.
- ResMed AirSense 10 AutoSet: This is a very popular and user-friendly auto-CPAP machine. It automatically adjusts pressure based on your breathing needs. It's known for its quiet operation and integrated humidifier.
- Philips Respironics DreamStation Auto CPAP: Another top contender, offering similar auto-adjusting features and quiet performance. It has a sleek design and user-friendly interface.
- Fisher & Paykel SleepStyle Auto CPAP: Known for its simple design and easy-to-clean humidifier. It's a good option for those who prefer straightforward operation.
Comparison: All three are excellent auto-CPAP machines. ResMed and Philips are often neck and neck in terms of features and user satisfaction. Fisher & Paykel offers a slightly more basic but reliable experience. The best choice often comes down to personal preference for interface, mask compatibility, and specific features like data tracking apps.
Typical Price Range: $800 - $1,500 USD (machine only, masks and accessories are separate).
CPAP Masks Comfort and Fit
The mask is just as important as the machine for CPAP therapy adherence. There are three main types:
- Nasal Masks: Cover the nose only. Good for those who breathe through their nose and prefer less facial contact. (e.g., ResMed AirFit N20, Philips DreamWear Nasal)
- Nasal Pillow Masks: Small cushions that fit directly into the nostrils. Minimal contact, great for claustrophobia or side sleepers. (e.g., ResMed AirFit P10, Philips DreamWear Nasal Pillows)
- Full Face Masks: Cover both the nose and mouth. Ideal for mouth breathers or those with nasal congestion. (e.g., ResMed AirFit F20, Philips DreamWear Full Face)
Comparison: Nasal pillow masks offer the most freedom but might not be suitable for high pressures. Full face masks provide the most secure seal but can feel bulkier. Nasal masks are a good middle ground. Trying different types is crucial to find the best fit and comfort.
Typical Price Range: $100 - $250 USD.
Oral Appliances for Mild to Moderate Sleep Apnea and Snoring
For mild to moderate sleep apnea or primary snoring, custom-made oral appliances can be an alternative to CPAP. These devices, fitted by a dentist, reposition the jaw or tongue to keep the airway open.
- Mandibular Advancement Devices (MADs): These devices gently push the lower jaw forward. (e.g., SomnoDent, Herbst Appliance)
- Tongue Retaining Devices (TRDs): Hold the tongue in a forward position. (e.g., AveoTSD)
Comparison: MADs are more common and generally more effective for sleep apnea. TRDs are simpler but might be less comfortable for some. Both require professional fitting.
Typical Price Range: $1,500 - $3,000 USD (custom-made, often covered by medical insurance).
Light Therapy Lamps for Circadian Rhythm Disorders
For conditions like Seasonal Affective Disorder (SAD) or circadian rhythm sleep-wake disorders (e.g., delayed sleep phase syndrome), light therapy lamps can be very helpful.
- Philips SmartSleep Wake-up Light: Combines a sunrise simulation alarm with light therapy. It gradually brightens to wake you naturally and can also be used for evening wind-down.
- Carex Day-Light Classic Plus: A popular and effective full-spectrum light therapy lamp, delivering 10,000 lux. It's a larger, more traditional light box.
- Verilux HappyLight Liberty Compact: A smaller, portable option for light therapy, also delivering 10,000 lux. Great for travel or smaller spaces.
Comparison: Philips offers a more integrated alarm clock experience. Carex and Verilux are dedicated light therapy devices. The key is to ensure they deliver 10,000 lux at a comfortable distance and are UV-filtered.
Typical Price Range: $50 - $200 USD.
White Noise Machines and Sound Machines for Sleep Environment
These devices create a consistent sound environment to mask disruptive noises, helping you fall asleep and stay asleep.
- LectroFan Evo: Offers 22 non-looping sounds, including white noise, fan sounds, and ocean sounds. Very effective and highly rated.
- Hatch Restore: A multi-functional device combining a sound machine, smart light, alarm clock, and meditation app. Great for creating a comprehensive sleep routine.
- Dohm Nova by Marpac: Uses a real fan to create natural, non-looping white noise. A classic choice for many.
Comparison: LectroFan is excellent for pure sound masking. Hatch Restore is a premium all-in-one solution for a complete sleep environment. Dohm Nova is a simple, effective, and durable option for natural white noise.
Typical Price Range: $30 - $130 USD.
Sleep Trackers and Smart Rings for Data Insights
While not diagnostic tools, these can provide valuable insights into your sleep patterns and help you track progress once you start treatment.
- Oura Ring Gen3: A highly accurate and discreet smart ring that tracks sleep stages, heart rate variability, body temperature, and activity. Provides personalized insights and readiness scores.
- Whoop 4.0: A wrist-worn strap focused on recovery, sleep, and strain. Offers detailed sleep stage tracking and recovery metrics.
- Fitbit Sense 2: A smartwatch with advanced sleep tracking features, including sleep stages, heart rate, and skin temperature. Also offers stress management tools.
Comparison: Oura Ring is known for its comfort and accuracy in sleep tracking, especially for sleep stages. Whoop is popular among athletes for its recovery focus. Fitbit is a versatile smartwatch with good general health and sleep tracking capabilities.
Typical Price Range: Oura Ring ($299 - $399 + subscription), Whoop ($30/month subscription), Fitbit Sense 2 ($299).
The Importance of Follow-Up Care Ongoing Sleep Health
Getting a diagnosis is just the beginning. Effective management of sleep disorders often requires ongoing follow-up care with your sleep specialist. This allows them to monitor your progress, adjust treatments as needed, and address any new concerns that arise. Regular check-ins ensure that you're getting the most out of your treatment and that your sleep health continues to improve. Remember, better sleep isn't just a luxury; it's a fundamental pillar of your overall health and well-being.
So, if you suspect you have a sleep disorder, don't delay. Reach out to a healthcare professional. Taking that first step towards diagnosis can truly be life-changing, paving the way for more restful nights and more energetic days.
:max_bytes(150000):strip_icc()/277019-baked-pork-chops-with-cream-of-mushroom-soup-DDMFS-beauty-4x3-BG-7505-5762b731cf30447d9cbbbbbf387beafa.jpg)